In this article
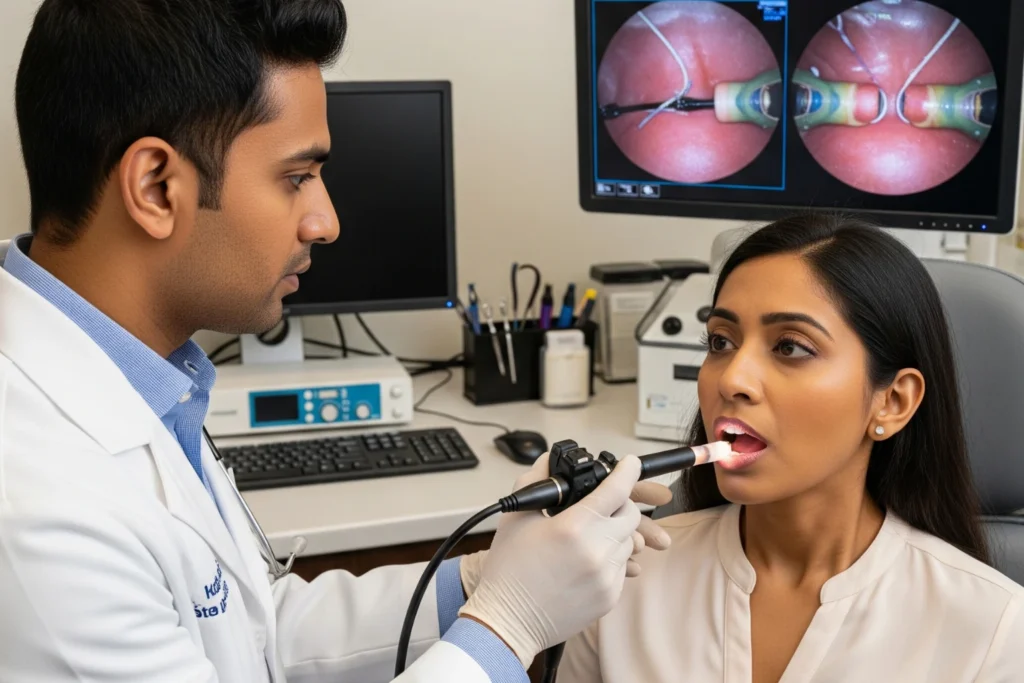
What is Vocal Cord Paralysis?
Your voice plays a vital role in how you communicate, express your emotions, and connect with the people around you. When you speak, two small bands of muscle tissue inside your windpipe come together and vibrate to create sound. Doctors call these bands the vocal cords (or vocal folds). They sit inside your voice box, which acts as a protective gateway for your airway. Beyond producing sound, your vocal cords perform a critical safety function every single day. They open wide when you breathe to let air into your lungs, and they snap tightly shut when you swallow to keep food and liquids out of your airway.
Vocal cord paralysis happens when the nerve impulses traveling to your voice box become disrupted. This nerve damage paralyzes the muscle of the vocal cord, preventing it from moving properly. The condition can affect just one vocal cord, which doctors call unilateral paralysis, or it can affect both sides, known as bilateral paralysis. Unilateral paralysis occurs much more frequently than bilateral paralysis. When one cord cannot move, the healthy cord cannot reach across to close the gap. This leaves your airway partially open, making your voice sound weak and allowing food or liquid to slip down into your lungs.
Sometimes, the nerve is only partially damaged, leading to a condition called vocal cord paresis (partial weakness). While paresis allows for some movement, complete paralysis means the vocal cord remains entirely frozen in place. Losing your voice can feel incredibly isolating, often impacting your career, your social life, and your emotional well-being. Many patients experience frustration and anxiety when people constantly ask them to repeat themselves or when they struggle to be heard in a noisy room.
In India, clinical studies show that vocal cord paralysis accounts for roughly 42 out of every 10,000 visits to ear, nose, and throat (ENT) specialists. The condition most commonly affects adults between the ages of 40 and 60. Interestingly, the left vocal cord suffers paralysis almost twice as often as the right side. This happens because the nerve controlling the left vocal cord takes a much longer journey through your chest cavity, exposing it to more potential injuries or diseases along the way. While a paralyzed vocal cord can feel frightening, modern medicine offers many effective solutions to restore your voice and protect your health.
Causes and Risk Factors
To understand what causes vocal cord paralysis, you must first understand how your brain communicates with your voice box. The vagus nerve travels from your brainstem down through your neck and into your chest. A specific branch of this nerve, called the recurrent laryngeal nerve, loops back up from the chest to control your vocal cords. Any injury, tumor, or infection anywhere along this long nerve pathway can paralyze the vocal cord.
Medical professionals categorize the causes of vocal cord paralysis into several main groups:
- Surgical Injury: Experiencing voice loss after surgery remains one of the most common causes of a paralyzed vocal cord. Because the recurrent laryngeal nerve runs very close to the thyroid gland, the heart, and the spine, operations in these areas carry a risk of nerve damage. Thyroid surgery, heart bypass surgery, and neck spine operations frequently cause this complication.
- Tumors and Growths: Both cancerous and non-cancerous tumors can grow around the nerve and compress it. Tumors in the thyroid gland, esophagus, lungs, or neck often press against the recurrent laryngeal nerve, stopping its signals.
- Viral Infections: Sometimes, a severe viral infection can attack the nerve directly, causing inflammation and damage. Doctors call this post-viral neuropathy. In many of these cases, the nerve eventually heals on its own, though recovery can take several months.
- Neurological Conditions: Diseases that affect the brain and nervous system can disrupt the signals sent to the voice box. Conditions like Parkinson's disease, multiple sclerosis, or a stroke can lead to vocal cord weakness or complete paralysis.
- Neck or Chest Trauma: A direct physical injury to the neck or chest, such as from a car accident, can sever or crush the nerve. Additionally, the breathing tubes used during general anesthesia or in intensive care units can sometimes bruise the vocal cords or the surrounding nerves.
Risk Factors Specific to Indian Patients
Certain environmental, dietary, and lifestyle factors make specific causes more prevalent among patients in India:
- Tuberculosis (TB): India carries a high burden of tuberculosis. TB can cause the lymph nodes in the chest to become severely enlarged. These swollen tubercular lymph nodes can press against the recurrent laryngeal nerve, leading to paralysis.
- Tobacco Use: The high rates of smoking and chewing tobacco (including gutka and paan) in India significantly increase the risk of head, neck, and lung cancers. These cancers frequently invade the nerve pathways that control the voice.
- Thyroid Disease: India has a large population dealing with goiters and thyroid nodules. The high volume of thyroid surgeries naturally increases the regional incidence of voice loss after surgery.
Signs and Symptoms
The symptoms of vocal cord paralysis range from mild voice changes to severe breathing and swallowing difficulties. The severity of your symptoms depends entirely on whether one or both cords are paralyzed, and the exact position where the paralyzed cord has stopped moving. When a vocal cord stops moving, it usually gets stuck in an open or half-open position. Because the cords cannot close completely, air escapes rapidly when you try to speak.
You will likely notice these early warning signs regarding your voice:
- A breathy, weak, or raspy voice quality
- Inability to speak loudly, project your voice, or shout
- Loss of your normal vocal pitch or singing range
- Feeling completely out of breath while talking
- A frequent, uncontrollable need to clear your throat
If you experience persistent voice changes, you might find helpful information in our guide on why hoarseness won't go away and when to see an ENT.
As the condition progresses, or if the gap between the vocal cords remains large, you may experience more serious symptoms related to swallowing and breathing. You may also notice that you cannot produce a strong cough. You need tightly closed vocal cords to build up chest pressure for a strong cough; without this pressure, you cannot clear phlegm from your chest effectively.
Watch for these severe progression signs:
- Aspiration: This occurs when food, liquids, or even your own saliva slip through the open vocal cords and enter your windpipe. You will experience sudden, violent coughing or choking when you try to eat or drink.
- Pneumonia: Frequent aspiration can carry mouth bacteria down into your lungs, leading to a serious chest infection called aspiration pneumonia.
- Noisy Breathing: If the vocal cords become paralyzed in a closed position, they block the airway. This causes a high-pitched wheezing sound when you breathe in, which doctors call stridor.
- Difficulty Swallowing: You may feel like food gets stuck in your throat, requiring you to swallow multiple times for a single bite.
See a Doctor If...
You should schedule an immediate evaluation if you experience unexplained hoarseness that lasts for more than two weeks. You must seek emergency medical care if you develop sudden difficulty breathing, noisy breathing, or if you frequently choke and cough when drinking water.

How is Vocal Cord Paralysis Diagnosed?
Accurate diagnosis requires a thorough examination of your voice box and the entire nerve pathway. When you visit the Laryngology department at THANC Hospital, our specialists will first listen carefully to your voice and ask detailed questions about your medical history. We will pay special attention to any recent surgeries, illnesses, or injuries that might explain your symptoms.
To confirm vocal cord paralysis and find its root cause, we use several advanced diagnostic tools:
- Endoscopic Laryngoscopy: During this routine clinic procedure, the doctor passes a thin, flexible tube with a tiny camera through your nose and down into your throat. This allows the doctor to watch your vocal cords in real-time as you speak and breathe. We apply a numbing spray to your nose beforehand, making the procedure quick and highly comfortable.
- Videostroboscopy: This specialized test uses a flashing strobe light connected to a camera. The strobe light flashes in sync with your voice, creating a slow-motion video of your vocal cords vibrating. During the test, the doctor will ask you to hold a steady "eee" sound. This helps the doctor see exactly how much of a gap remains when you try to close your vocal cords.
- Imaging Scans: Because the nerve travels all the way through your neck and chest, we must look for any hidden tumors, enlarged lymph nodes, or injuries along that path. Your doctor will likely order a Computed Tomography (CT) scan or Magnetic Resonance Imaging (MRI) of your brain, neck, and upper chest.
- Laryngeal Electromyography (LEMG): Think of this test like an ECG for your voice box muscles. The doctor inserts a tiny needle through the skin of your neck into the vocal cord muscles to measure their electrical currents. By measuring these electrical signals, we can determine the exact extent of the nerve damage and predict how well the nerve might recover on its own.
Knowing what to expect during these tests can help reduce your anxiety. Our team so that every diagnostic step remains as comfortable and informative as possible. We always explain the results to you immediately, showing you the images of your vocal cords on our clinic viewing screens.
Treatment Options
The treatment for vocal cord paralysis depends on the underlying cause, the severity of your symptoms, and how long you have had the condition. Our primary goals are to improve your voice quality, prevent choking, and ensure you can breathe safely. We generally divide treatments into conservative management and surgical interventions.
Conservative and Medical Management
If a viral infection caused your paralysis, or if you recently experienced voice loss after surgery, your doctor may recommend waiting before trying surgery. Nerves heal very slowly, and your vocal cord may regain movement naturally within six to twelve months. During this waiting period, we focus on protecting your airway and maximizing your current voice.
- Voice Therapy: A speech-language pathologist will teach you specific exercises to strengthen your healthy vocal cord. You will learn how to use your breath more efficiently and how to protect your airway when you swallow.
- Dietary Modifications: If you struggle with choking, we may recommend thickening your liquids or changing the texture of your food to make swallowing safer.
Surgical Options
If your voice does not return, or if you face a high risk of aspiration pneumonia, we will recommend surgery. The goal of surgery is to push the paralyzed vocal cord toward the middle of your airway. This allows the healthy cord to meet the paralyzed one, closing the gap effectively.
- Vocal Cord Injection (Medialization): The doctor injects a plumping substance directly into the paralyzed vocal cord to add bulk. We can use temporary materials, like hyaluronic acid, which last a few months while we wait to see if the nerve heals. For a permanent solution, we can inject your own body fat or specialized medical gels.
- Thyroplasty: This permanent surgical procedure involves making a small incision in your neck. The surgeon creates a tiny window in your voice box cartilage and inserts a custom-shaped implant. This implant permanently pushes the paralyzed cord into the correct position.
- Arytenoid Adduction: Surgeons often perform this procedure alongside a thyroplasty. The surgeon places a small stitch to rotate the cartilage at the back of the vocal cord, helping to close the gap even more tightly.
- Laryngeal Reinnervation: In this complex procedure, the surgeon takes a healthy nerve from another part of your neck and connects it to the paralyzed vocal cord muscle. While this does not restore normal movement, it keeps the muscle healthy and provides excellent voice quality over time.
- Tracheostomy: If you suffer from bilateral vocal cord paralysis, both cords may lock in the closed position, blocking your airway. In this life-threatening emergency, the surgeon must create a small hole in the front of your neck directly into your windpipe to help you breathe.
At THANC Hospital, we use modern surgical approaches, including Transoral Laser Microsurgery (TLM) and Transoral Robotic Surgery (TORS), to treat complex laryngeal conditions with precision and minimal recovery time.
Living with Vocal Cord Paralysis / Recovery and Outlook
Recovering from vocal cord paralysis requires patience and active participation in your daily care. If you undergo a vocal cord injection or thyroplasty, you will likely notice an immediate improvement in your voice and your ability to swallow safely. However, your throat may feel sore for a few days, and you will need to rest your voice strictly as directed by your surgeon.
Living with a paralyzed vocal cord means paying close attention to your vocal hygiene and swallowing habits. You must stay well-hydrated by drinking plenty of water throughout the day. Dry vocal cords require much more effort to vibrate, which can severely strain your healthy vocal cord. Overworking your healthy cord to compensate for the paralyzed one can sometimes lead to secondary issues, which you can read more about in our article on vocal cord nodules and polyps.
You should also actively manage any acid reflux. Stomach acid that travels up into your throat can severely irritate a paralyzed vocal cord, causing swelling and further voice deterioration. Learn how to protect your throat by reading our guide on laryngopharyngeal reflux (silent reflux).
To ensure safe swallowing at home, practice the "chin-tuck" method during meals. When you take a sip of liquid, tuck your chin down toward your chest before you swallow. This simple physical movement changes the angle of your throat and helps close off your airway, preventing choking. You may also need to practice vocal pacing at work, taking frequent breaks to rest your voice during long meetings or phone calls.
Your follow-up care will involve regular visits to the laryngologist and speech therapist. We will monitor your voice quality, check for any signs of lung infections, and ensure your swallowing remains safe and effective for the long term.
Why Choose THANC Hospital for Vocal Cord Paralysis?
When dealing with complex voice and airway disorders, the experience of your surgical team makes a important difference in your recovery. At THANC Hospital, Dr. Vidhyadharan S has deep specialized training in Laryngology, Head & Neck Surgical Oncology, and Microvascular Reconstructive Surgery. His deep understanding of the intricate nerve pathways in the neck delivers precise diagnosis and highly targeted treatment plans.
Our hospital combines a team-based approach, bringing together expert laryngologists, speech-language pathologists, and specialized imaging technicians under one roof. We focus on preserving your voice and protecting your quality of life using the most effective, minimally invasive techniques available today. If you are struggling with voice changes or swallowing difficulties, we encourage you to Book an Appointment for a thorough evaluation.
Frequently Asked Questions
Can vocal cord paralysis heal on its own?
Yes, in some cases, the nerve can heal naturally without surgical intervention. This spontaneous recovery most often happens when a viral infection or minor surgical bruising causes the paralysis. However, the healing process moves slowly and can take anywhere from six months to a full year.
How long does voice loss after surgery last?
Voice loss after surgery can be temporary or permanent, depending on whether the nerve was simply bruised or completely severed. If the nerve only suffered stretching or bruising during the operation, your voice may gradually return over several months. If the surgeon had to cut the nerve to remove a tumor, the voice loss will be permanent without corrective surgery.
Is vocal cord paralysis life-threatening?
Unilateral paralysis (affecting one side) is rarely life-threatening, though it can cause severe pneumonia if food and liquids constantly enter your lungs. However, bilateral paralysis (affecting both sides) can become a life-threatening emergency. If both vocal cords paralyze in the closed position, they block your windpipe and prevent you from breathing.
What foods should I avoid if I have trouble swallowing?
If you experience choking, you should avoid thin liquids like plain water, tea, or clear broth, as these slip into the airway very easily. You should also avoid dry, crumbly foods like crackers or nuts that can scatter in your throat. Stick to soft, moist foods and consider using commercial thickeners to make liquids safer to swallow.
Does speech therapy really help a paralyzed vocal cord?
Yes, speech therapy plays a vital role in your recovery process. A speech-language pathologist will teach you specific exercises to strengthen your healthy vocal cord so it can compensate for the paralyzed one. Therapy also teaches you important techniques to swallow safely and prevent food from entering your lungs.
How successful is surgery for a paralyzed vocal cord?
Surgical procedures like vocal cord injections and thyroplasty have very high success rates for restoring a strong, functional voice. Most patients experience immediate improvement in their ability to speak loudly and swallow safely right after the procedure. While your voice may not sound exactly as it did before the paralysis, surgery significantly improves your daily communication and quality of life.
Learn more about Laryngology
View treatments, doctors & FAQs
Concerned about this condition?
Our specialists can help. Book a consultation today.
Book Consultation