In this article

Swallowing Problems After Stroke — What You Need to Know
A stroke changes life in an instant, affecting movement, speech, and memory. However, one of the most common and dangerous complications happens entirely out of sight. Many stroke survivors lose the ability to swallow food and liquids safely. This condition requires immediate attention to prevent severe health complications and ensure a safe recovery.
dysphagia (difficulty swallowing) affects nearly 45% of all stroke patients. In India, stroke incidence is rising rapidly, with studies showing 119 to 145 cases per 100,000 people every year. High rates of hypertension and diabetes in the Indian population contribute heavily to this growing health burden. As more people survive strokes, the need for effective rehabilitation becomes critical for long-term survival.
Why does this guide matter? Swallowing problems do more than just make meals difficult. When the swallowing muscles fail to coordinate, food and liquids can slip into the windpipe instead of the stomach. This leads to a life-threatening lung infection. Furthermore, the fear of choking often causes patients to eat less, leading to severe malnutrition and dehydration. Proper difficulty swallowing management is essential for protecting the patient's overall health.
This guide is for stroke survivors, their families, and caregivers. Recovering from a stroke is a team effort, and family support plays a massive role in Indian households. Understanding how to manage meals, practice exercises, and navigate the recovery timeline will empower you to protect your loved one. With the right approach to swallowing rehab, patients can regain their strength, enjoy their meals safely, and significantly improve their quality of life.
Understanding Swallowing Problems After Stroke
To understand why a stroke affects swallowing, you must first understand how a normal swallow works. Swallowing is a complex process that requires the precise coordination of 50 pairs of muscles and many nerves. The brain acts as the control center, sending rapid-fire signals to the mouth, throat, and food pipe. When a stroke damages the parts of the brain that control these muscles, the communication breaks down.
The swallowing process happens in three distinct phases. First is the oral phase, where you chew food and mix it with saliva to form a cohesive ball. Second is the pharyngeal phase, where the throat muscles push the food down while the airway closes to protect the lungs. Finally, the esophageal phase moves the food down the food pipe and into the stomach. A stroke typically disrupts the first two phases, making it hard to chew or causing a dangerous delay in closing the airway.
When the airway does not close in time, food, liquid, or saliva enters the lungs. Medical professionals call this aspiration. This is highly dangerous because the lungs cannot clear these food particles, which quickly breed bacteria. This results in aspiration pneumonia, a severe infection that remains a leading cause of death in stroke survivors.
Sometimes, a patient may inhale food or liquid into their lungs without coughing or showing any outward signs of distress. Doctors refer to this as silent aspiration. Because the stroke damages the sensory nerves in the throat, the patient does not feel the liquid entering the wrong pipe. This makes silent aspiration incredibly dangerous, as caregivers may assume the patient is eating safely when they are actually at high risk.
The severity of dysphagia after stroke depends heavily on the location and size of the brain injury. Strokes occurring in the brainstem often cause the most severe swallowing deficits, as the brainstem directly houses the swallowing center. However, strokes in the cerebral cortex can also cause significant problems, particularly with chewing and moving food to the back of the mouth. Understanding these mechanics helps explain why recovery takes time and requires targeted therapy.
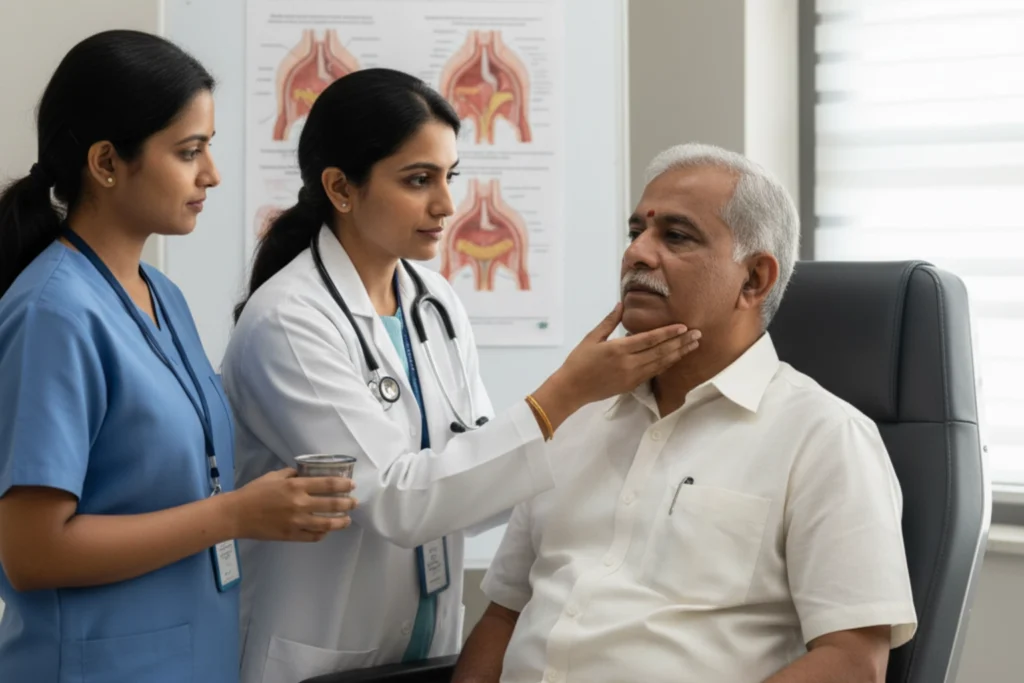
Step-by-Step Guide
Recovering your swallowing ability requires a structured, step-by-step approach. You cannot rush this process, as eating the wrong foods too early can lead to serious lung infections. A dedicated swallowing rehab program focuses on safety first, followed by muscle strengthening and coordination. Here is the standard pathway for managing and treating swallowing problems after a stroke.
Step 1: Full Swallowing Assessment Before you eat or drink anything, a specialist must evaluate your swallowing function.
- Bedside Swallow Evaluation: A specialist will observe you swallowing small amounts of water or pureed food. They will check for coughing, voice changes, or difficulty clearing the mouth.
- Instrumental Testing: If the bedside test shows risks, you will need advanced imaging. The Flexible Endoscopic Evaluation of Swallowing (FEES) uses a tiny camera passed through the nose to watch the throat during a swallow.
- Videofluoroscopic Swallow Study (VFSS): Also known as a modified barium swallow, this is a moving X-ray that tracks food from the mouth to the stomach. These tests identify silent aspiration and determine exactly which phase of swallowing is failing.
Step 2: Dietary Modifications Until your muscles regain their strength, you must change the texture of your food and liquids. Thin liquids move very quickly and are the hardest to control, making them the most likely to enter the lungs.
- Thickened Liquids: You may need to add commercial thickeners to water, tea, or milk. The consistency might need to be like mango nectar or even as thick as honey.
- Avoiding Dangerous Indian Staples: Thin, watery dishes like rasam, clear soups, or thin dals pose a high choking risk. You must avoid these until your specialist clears you.
- Pureed and Soft Diets: Transition to foods that require little to no chewing. Mashed idli soaked in thick sambar, blended khichdi, or smooth upma are excellent options. Avoid foods with mixed textures, like cereal with milk, because the brain struggles to handle a liquid and a solid at the same time.
Step 3: Targeted Swallowing Exercises Just like you need physical therapy for a weak arm or leg, you need swallowing rehab for your throat muscles. Your specialist will teach you specific exercises to rebuild neural pathways and muscle strength.
- Effortful Swallow: Swallow as hard as you can, squeezing all the muscles in your throat and neck. This helps push food completely through the throat, leaving no residue behind.
- Mendelsohn Maneuver: Place your fingers on your Adam's apple and swallow. Notice how it moves up and down. Now, swallow again and hold your Adam's apple up at its highest point for two to three seconds before relaxing. This keeps the airway protected longer.
- Shaker Exercise: Lie flat on your back without a pillow. Lift just your head to look at your toes while keeping your shoulders flat on the bed. Hold this position to strengthen the muscles that open the food pipe.
- Masako Maneuver: Stick your tongue out gently between your teeth and hold it there while you swallow your saliva. This forces the muscles in the back of your throat to work harder.
Step 4: Postural Adjustments During Meals Changing the position of your head and body can drastically improve swallowing safety. These simple adjustments change the path that food takes, using gravity to your advantage.
- Chin Tuck: Tuck your chin down to your chest right before you swallow. This posture physically narrows the airway opening, making it harder for food to enter the lungs.
- Head Turn: If the stroke weakened one side of your throat, turn your head toward the weak side while swallowing. This blocks off the weak side and forces the food down the stronger, functioning side of your throat.
- Upright Seating: Always sit at a strict 90-degree angle while eating. Never eat while lying down or reclining in bed.
Step 5: Alternative Feeding Methods In some cases, the swallowing muscles are too weak to safely consume enough calories by mouth. When this happens, your medical team will recommend a temporary feeding tube.
- Nasogastric (NG) Tube: A thin tube passes through the nose, down the throat, and into the stomach. This is usually a short-term solution for the first few weeks.
- PEG Tube: If recovery takes longer, a doctor may place a tube directly into the stomach through the abdomen. This is more comfortable than a nose tube and can be hidden under clothing.
- Important Note: Relying on a feeding tube does not mean you have failed. It simply gives you receive proper nutrition and hydration while you focus your energy on swallowing rehab.
What to Expect
The journey to regain swallowing function varies wildly from person to person. Understanding the recovery timeline helps manage expectations and reduces frustration. The brain possesses a remarkable ability called neuroplasticity, which allows healthy brain cells to take over the functions of the damaged cells. However, this rewiring process takes consistent practice and time.
During the acute phase, which covers the first two to four weeks after the stroke, you will see the most rapid changes. Many patients experience spontaneous recovery during this window as the initial swelling in the brain goes down. If you have mild dysphagia after stroke, you might return to a near-normal diet within a month. However, you must still follow your specialist's guidelines strictly during this vulnerable period.
If your swallowing difficulties persist beyond the first month, you enter the subacute and chronic phases of recovery. Progress during this time becomes slower and requires intense, daily swallowing rehab. You might spend several months working with a specialist to upgrade your diet from pureed foods to soft solids. Some patients may always need to drink slightly thickened liquids or use specific head postures to eat safely.
You will face several common challenges during this journey. Frustration and depression are incredibly common, as meals shift from a joyful family activity to a stressful medical task. You might also experience a fear of choking, which can cause you to lose your appetite entirely. Caregivers must remain patient, offer emotional support, and celebrate small victories, like successfully drinking a glass of nectar-thick water without coughing.
Weight loss is another significant challenge during recovery. Because eating takes so much effort and time, patients often consume fewer calories than their bodies need to heal. Caregivers should monitor the patient's weight weekly and report any sudden drops to the medical team. You may need to incorporate high-calorie nutritional supplements into the modified diet to keep energy levels up.
Tips for Better Outcomes
Achieving the best possible recovery requires more than just doing your exercises. Your daily habits, mealtime environment, and oral hygiene play a massive role in your success. Implementing these practical tips from clinical experience will keep you safe and accelerate your progress.
Create a Safe Mealtime Environment
- Eliminate Distractions: Turn off the television, put away mobile phones, and avoid complex conversations during meals. Swallowing now requires your full, conscious attention.
- Take Small Bites: Use a teaspoon instead of a tablespoon to control the amount of food entering your mouth. Smaller portions are much easier for weak muscles to manage.
- Eat Slowly: Put your spoon down between every bite. Wait until your mouth is completely clear before taking the next bite. Rushing leads to fatigue and increases the risk of choking.
- Stay Upright: Remain sitting upright at a 90-degree angle for at least 30 to 45 minutes after finishing your meal. This prevents food or stomach acid from coming back up into your throat.
Do's and Don'ts for Stroke Survivors
- Do perform your swallowing exercises daily, exactly as prescribed by your specialist. Consistency is the key to neuroplasticity.
- Do alternate between bites of solid food and sips of thickened liquid to help wash down any food stuck in your throat.
- Do check your mouth after eating. Stroke survivors often pocket food in the cheeks on their weak side without realizing it. Use your finger or tongue to sweep the mouth clean.
- Don't use a straw unless specifically instructed by your specialist. Straws shoot liquid to the back of the throat faster than your muscles can react.
- Don't wash down pills with water if you are on a thickened liquid diet. Ask your doctor if your medications can be crushed and mixed with applesauce or yogurt.
Focus on Aggressive Oral Hygiene Good oral care is one of the most effective ways to prevent aspiration pneumonia. Even if you are not eating by mouth and rely on a feeding tube, bacteria constantly build up in your saliva. If you aspirate that bacteria-filled saliva, you can develop a severe lung infection. Brush your teeth, gums, and tongue at least twice a day. If you cannot spit, caregivers should use a suction toothbrush or a damp gauze pad to clean the mouth safely.
Adapt to Indian Dietary Needs Indian meals often feature complex textures that are dangerous for stroke survivors. Dishes that mix liquids and solids, like cereal in milk or rasam with rice, confuse the swallowing mechanism. Instead, blend your meals to a uniform consistency. Spices can also trigger coughing fits, which disrupt the swallowing sequence. Keep your meals mildly spiced during the early stages of recovery. Additionally, ensure food is served at a moderate temperature, as extremely hot or cold foods can shock sensitive throat tissues.
When to Seek Medical Help
Even with the best care and strict adherence to a swallowing rehab program, complications can arise. You must monitor the stroke survivor closely for any signs that their swallowing function is deteriorating or that an infection is developing. Catching these warning signs early can prevent a hospital readmission and save a life.
Watch closely for signs of aspiration during or immediately after meals. If the patient coughs, chokes, or clears their throat frequently while eating, their current diet texture may be too difficult for them. Another major red flag is a "wet" or gurgly sounding voice after taking a drink. This sound indicates that liquid is sitting on top of the vocal cords, dangerously close to the lungs. If you notice these signs, stop feeding immediately and contact your specialist.
Aspiration pneumonia can develop silently, especially in patients who do not cough when food enters their lungs. You must watch for systemic signs of infection. If the patient develops a recurring low-grade fever, sudden shortness of breath, or a sharp pain in their chest, seek emergency medical care immediately. Increased confusion, extreme fatigue, or a sudden change in mental status can also indicate an underlying infection in older stroke survivors.
Finally, seek professional help if self-management at home isn't working. If the patient refuses to eat, experiences unexplained weight loss, or shows signs of severe dehydration like dark urine and dry mouth, you need medical intervention. The medical team can adjust the diet, provide intravenous fluids, or discuss temporary tube feeding options to stabilize the patient's health.
Expert Care at THANC Hospital
At THANC Hospital, our Swallowing Disorders Clinic provides specialized care for stroke survivors struggling with dysphagia. Under the expert guidance of Dr. Vidhyadharan S, our team uses advanced diagnostic tools like FEES to create your rehabilitation plans. If you or a loved one is facing swallowing difficulties after a stroke, Book an Appointment today to start a safe and effective recovery journey.
Frequently Asked Questions
Can swallowing problems after a stroke be cured completely?
Many patients regain their normal swallowing ability, especially if the stroke was mild and they start rehabilitation early. However, recovery depends on the severity and location of the brain injury. Some patients may always need minor dietary modifications or specific swallowing techniques to eat safely.
How long does it take to recover swallowing after a stroke?
The fastest improvement usually happens in the first two to four weeks as brain swelling decreases. For more severe strokes, recovery can take several months of dedicated daily exercises. Consistent therapy is important for retraining the brain and strengthening the throat muscles.
Why does my loved one cough when drinking water but not when eating solid food?
Thin liquids like water move very quickly, requiring fast reflexes to close the airway in time. A stroke often slows down these reflexes, allowing the water to slip into the windpipe and trigger a cough. Solid foods move slower, giving the brain and muscles more time to coordinate a safe swallow.
Is it safe to give a stroke patient regular tea or coffee?
If the patient has been prescribed thickened liquids, regular tea or coffee is not safe because it is too thin. You must add a commercial thickening powder to the beverage to reach the consistency recommended by your specialist. Always follow the exact dietary guidelines provided by your medical team.
What should I do if the patient refuses to eat pureed food?
Frustration with modified diets is very common. Try to improve the visual appeal and taste of the food by using food molds or adding mild, safe flavorings. If they continue to refuse food, consult your medical team, as they may need temporary nutritional support to prevent weight loss.
How do I know if the swallowing exercises are working?
You will notice gradual improvements, such as less coughing during meals, a clearer voice after drinking, and the ability to finish meals faster. Your specialist will also perform follow-up instrumental tests, like a swallow study, to objectively measure your progress and safely upgrade your diet.
Learn more about Swallowing Disorders Clinic
View treatments, doctors & FAQs
Concerned about this condition?
Our specialists can help. Book a consultation today.
Book Consultation
MBBS, MS (ENT), DNB (ENT), MCh (Head & Neck), FICRS, FEB – ORL HNS, ASOHNS
Clinical Director & Senior Consultant Surgeon