In this article
- What is Head & Neck Reconstruction — Free Flap & Microvascular Surgery?
- Who Needs Head Neck Reconstruction Surgery?
- How Free Flap Reconstruction is Performed
- Preparing for the Procedure
- Recovery After Free Flap Reconstruction
- Risks and Complications
- Results and Success Rate
- Why Choose THANC Hospital for Head Neck Reconstruction Surgery?
- Frequently Asked Questions
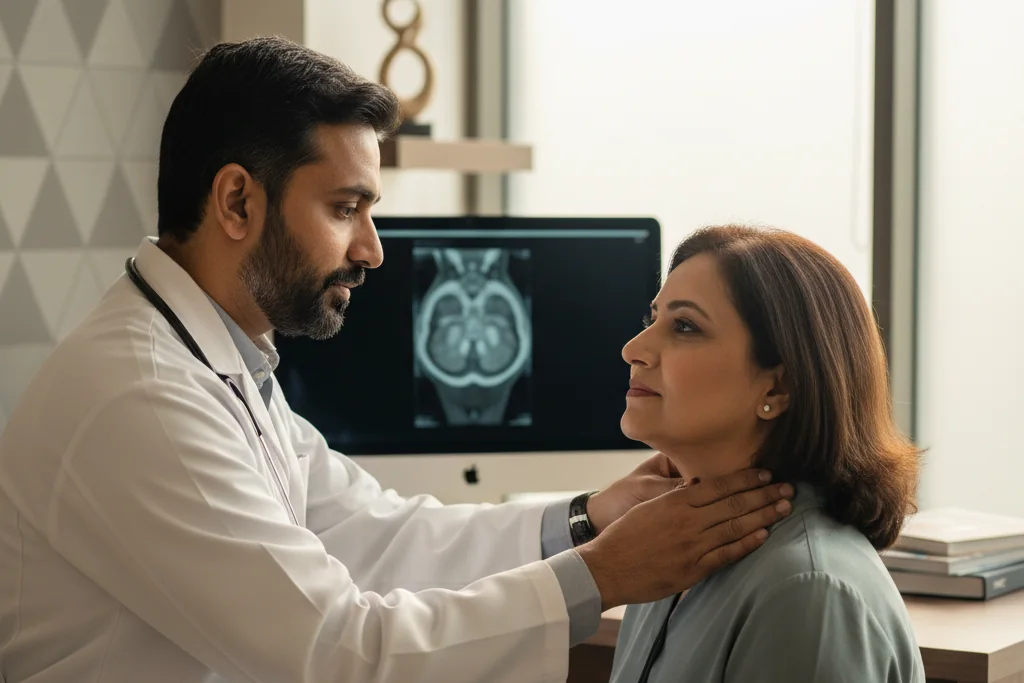
What is Head & Neck Reconstruction — Free Flap & Microvascular Surgery?
When you undergo surgery to remove a tumor from your mouth, jaw, face, or throat, the surgeon must take out the cancer along with a margin of healthy tissue. This process often leaves a significant gap or defect. Head neck reconstruction surgery aims to rebuild these missing parts, restore your appearance, and help you regain essential functions like breathing, chewing, swallowing, and speaking.
The most advanced and effective method to rebuild these complex areas is free flap reconstruction. In simple terms, a "flap" is a piece of living tissue—which can include skin, fat, muscle, or even bone—taken from one part of your body to repair another. The term "free" means the surgeon completely detaches this tissue from its original location, along with its blood supply.
Once the surgeon moves the tissue to your head or neck, they must reconnect the tiny blood vessels of the flap to the blood vessels in your neck. Because these blood vessels are often only one to two millimeters wide, the surgeon performs this delicate task under a high-powered microscope. This specific technique is called microvascular surgery.
By restoring a continuous blood supply, the transplanted tissue stays alive and heals naturally in its new location. This procedure solves major structural problems that simpler surgeries cannot fix. It allows surgeons to rebuild a missing jawbone, create a new tongue, or replace large areas of skin on the face and neck.
Without this specialized surgery, patients with large tissue defects would face severe difficulties with basic daily activities. Free flap reconstruction provides a permanent, living tissue replacement that integrates smoothly with your body over time.
Who Needs Head Neck Reconstruction Surgery?
Patients who require extensive removal of tissue in the head and neck region are the primary candidates for this procedure. In India, head and neck cancers account for nearly 30% of all cancer cases. This high prevalence is strongly linked to the widespread use of smokeless tobacco, betel quid (paan), and smoking.
Because many patients in India seek medical help at an advanced stage, surgeons often need to remove large portions of tissue to clear the disease completely. You can learn more about identifying these issues early in our guide on oral cancer early signs and symptoms.
You may need a free flap reconstruction if you face any of the following conditions:
- Advanced oral cavity cancers that require the removal of the jawbone, tongue, or cheek.
- Throat cancers that involve removing parts of the voice box or swallowing passages, which you can read about in our throat cancer types, stages, and treatment article.
- Severe facial trauma or accidents that result in massive tissue loss.
- Osteoradionecrosis, a condition where previous radiation therapy causes the jawbone to die and crumble.
- Congenital deformities (birth defects) that affect the structure of the face and skull.
Conservative treatments, such as stitching the wound edges together (primary closure) or using thin skin grafts, work well for very small defects. However, these simple methods fail when you lose a large volume of muscle or a segment of bone. A skin graft cannot replace a missing jawbone, and simple stitches cannot rebuild a functioning tongue. For a deeper understanding of tongue procedures, see our post on tongue cancer diagnosis, surgery, and recovery.
Ideal candidates for microvascular surgery are patients who have a good overall health status. Because the surgery takes many hours, your heart and lungs must be strong enough to handle prolonged anesthesia. You also need healthy blood vessels in the donor areas (like your legs or arms) to ensure the flap has a reliable blood supply.
How Free Flap Reconstruction is Performed
Free flap reconstruction is a complex, highly coordinated operation that involves multiple steps. A team of specialized surgeons works together to ensure the cancer is completely removed and the area is perfectly rebuilt. The entire procedure takes place under general anesthesia, meaning you will be completely asleep and pain-free.
The surgery generally lasts between 8 to 14 hours, depending on the size of the defect and the type of tissue needed. Because of the extensive nature of the operation, you can expect a hospital stay of about 10 to 14 days. This duration includes time spent in the intensive care unit for close monitoring.
The procedure follows four main steps:
Step 1: Tumor Removal (Ablation) The surgical oncology team begins by carefully removing the tumor and a safe margin of surrounding healthy tissue. They may also remove lymph nodes in your neck to prevent the cancer from spreading. Once they confirm the cancer is clear, they measure the exact size and shape of the resulting defect.
Step 2: Flap Harvesting While one team works on your neck, another surgical team carefully removes the required tissue from the donor site. The choice of donor site depends on what needs replacing:
- Fibula free flap: The surgeon takes a piece of bone from your lower leg to rebuild a missing jaw.
- Radial forearm free flap: The surgeon takes thin, pliable skin from your inner arm to rebuild a tongue or the inside of your cheek.
- Anterolateral thigh flap: The surgeon takes thicker skin and muscle from your thigh to fill large, deep spaces in the neck or face.
Step 3: Microvascular Anastomosis This is the most critical part of the head neck reconstruction surgery. The surgeon places the harvested tissue into the defect in your head or neck. Using a powerful microscope and stitches thinner than a human hair, the surgeon connects the artery and vein of the flap to an artery and vein in your neck. This restores blood flow and brings the new tissue to life.
Step 4: Insetting and Closure Once the blood flows smoothly through the new tissue, the surgeon shapes the flap to fit the defect perfectly. They secure the tissue in place with sutures or small titanium plates and screws if bone is involved. Finally, the surgical team carefully closes the donor site on your arm or leg, sometimes using a small skin graft to help it heal.
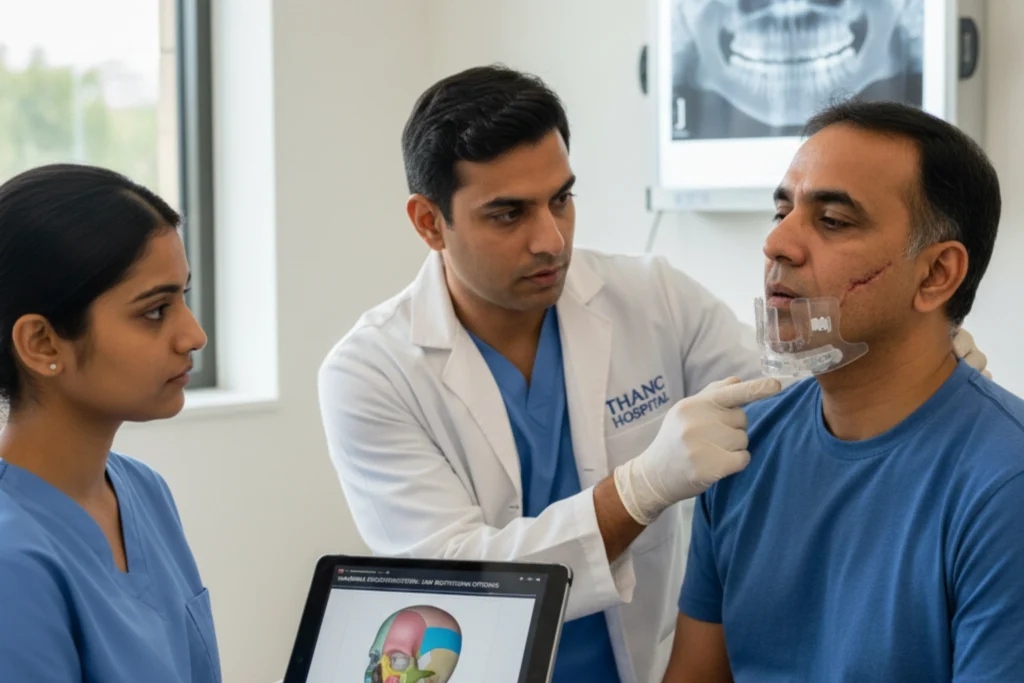
Preparing for the Procedure
Proper preparation is vital for the success of a free flap reconstruction. Your medical team will guide you through a series of steps to ensure your body is ready for a long surgery and a smooth recovery.
You will undergo several pre-operative tests to check your overall health. These typically include full blood tests, an electrocardiogram (ECG) to check your heart rhythm, and an echocardiogram to assess your heart function. If the surgeon plans to take bone from your leg, you will also need a CT angiography. This special scan maps out the blood vessels in your legs to ensure they are healthy enough to use.
Your doctor will give you strict instructions on what to stop and start before the surgery. You must follow these rules carefully:
- Stop smoking and chewing tobacco immediately. Nicotine shrinks blood vessels and drastically increases the risk of flap failure.
- Stop taking blood thinners, aspirin, and certain herbal supplements at least a week before surgery to prevent excessive bleeding.
- Start eating a high-protein diet to build up your nutritional reserves, which will help your wounds heal faster after the operation.
On the day of the surgery, you must arrive at the hospital with an empty stomach, usually fasting from midnight the night before. Bring comfortable, loose-fitting clothes, your personal toiletries, and all your medical records. You will meet with the anesthesia team, who will explain how they will keep you asleep and monitor your vital signs throughout the long operation.
Recovery After Free Flap Reconstruction
The recovery process requires patience, as your body needs time to heal both the head and neck area and the donor site. Your medical team will support you through every stage of this journey.
The First 24 to 48 Hours Immediately after surgery, you will move to the Intensive Care Unit (ICU). The nursing staff will check the blood flow to your new flap every hour using a handheld Doppler ultrasound device. This close monitoring supports the microvascular connections remain open and healthy.
During this time, you will likely have a tracheostomy tube in your neck to help you breathe safely while your airway is swollen. You will also receive nutrition and medications through a nasogastric tube (Ryles tube) that runs through your nose into your stomach. You will not be able to speak or eat by mouth for the first few days.
Week-by-Week Recovery Timeline
- Week 1: You will move from the ICU to a regular hospital room. The physical therapy team will help you sit up and take your first steps. Early movement prevents blood clots in your legs and helps your lungs expand.
- Week 2: As the swelling in your throat goes down, the doctor will usually remove the breathing tube. You will undergo a swallowing test. If the test shows you can swallow safely, you will start drinking clear liquids. The team will also remove your surgical drains.
- Weeks 3 to 4: You will likely be resting at home by this time. Your donor site (arm or leg) will continue to heal. You will transition from a liquid diet to soft, mashed foods. You must avoid strenuous activities and heavy lifting.
- Months 2 to 3: You will work closely with a speech and swallowing therapist to regain your normal functions. Your energy levels will slowly return to normal, and you can gradually resume your regular daily activities.
Diet and Activity Restrictions Your diet will progress slowly to protect the healing tissues in your mouth and throat. You must stick to soft, non-spicy foods for several weeks. Indian diets can be easily adapted by consuming well-mashed khichdi, soft idlis soaked in sambar, and pureed vegetables. You must avoid hard, crunchy, or very spicy foods that could irritate the surgical site.
Regarding physical activity, you should take short walks daily to build stamina. However, you must avoid bending over, lifting anything heavier than two kilograms, or engaging in vigorous exercise for at least six to eight weeks.

Risks and Complications
Like any major operation, free flap reconstruction carries certain risks. Your surgical team takes extensive precautions to minimize these issues, but you should understand what to watch for during your recovery.
Common and Minor Risks Minor complications occur more frequently but are generally easy to treat. You may experience minor wound infections, which respond well to antibiotics. Sometimes, fluid collects under the skin at the surgical site, a condition known as a seroma. The doctor can easily drain this fluid in the clinic. You may also experience temporary numbness, stiffness, or delayed healing at the donor site on your arm or leg.
Rare but Serious Risks The most serious risk is flap failure. This happens if a blood clot forms in the newly connected artery or vein, stopping the blood supply to the transplanted tissue. If the nurses detect a drop in blood flow during their hourly checks, the surgeon will take you back to the operating room immediately to clear the blockage. Severe bleeding and breathing difficulties are other rare but serious risks that require prompt medical attention.
How THANC Hospital Minimizes Risks Our hospital follows strict safety protocols to protect you. We minimize risks by carefully selecting patients, conducting thorough pre-operative testing, and using highly trained surgical teams. Our dedicated post-operative ICU staff monitors your flap continuously, allowing us to catch and treat any potential issues before they become serious problems.
Results and Success Rate
Free flap reconstruction is a highly reliable procedure. In experienced hands, the success rate for flap survival is between 90% and 95%. When the flap heals successfully, the results are permanent. The transplanted tissue becomes a living, integrated part of your head and neck.
The functional outcomes depend on the size and location of your original tumor. Most patients successfully regain their ability to eat by mouth, speak clearly, and breathe without assistance. While your speech or swallowing might feel different than it did before the cancer, dedicated rehabilitation therapy helps you maximize your function.
Aesthetically, the surgeon carefully designs the flap to match the natural contours of your face and neck as closely as possible. Over time, the swelling subsides, and the scars fade, helping you feel more comfortable and confident in your appearance.
Why Choose THANC Hospital for Head Neck Reconstruction Surgery?
When facing complex cancer treatment, choosing the right medical team makes all the difference. At THANC Hospital, our Head & Neck Surgery department handles a high volume of complex microvascular cases, giving our team the deep experience required for successful outcomes.
Dr. Vidhyadharan S specializes in Head & Neck Surgical Oncology and Microvascular Reconstructive Surgery. Our team-based approach so that your cancer removal, reconstruction, and rehabilitation are smoothly coordinated under one roof. If you or a loved one needs expert care, you can easily Book an Appointment to discuss your treatment options with our specialists.
Frequently Asked Questions
How painful is the donor site after surgery?
The donor site on your arm or leg will feel sore and tight for the first few weeks. Most patients find that the donor site actually causes more discomfort initially than the head and neck area. Your medical team will provide effective pain medications to keep you comfortable while you heal.
Will I have permanent scars on my face or neck?
Yes, the surgery will leave scars where the surgeon makes the incisions to remove the tumor and place the flap. However, the surgeon carefully places these incisions in the natural creases of your neck and face whenever possible. Over several months, these scars will fade and become much less noticeable.
How long will I need the feeding tube?
Most patients rely on a feeding tube for about two to three weeks after surgery. The exact time depends on how quickly your mouth and throat heal and how well you perform on your swallowing tests. Once you can safely swallow liquids and soft foods without choking, the doctor will remove the tube.
Can the transplanted bone in my jaw support dental implants?
Yes, if the surgeon uses bone from your leg (fibula) to rebuild your jaw, that bone is strong enough to support dental implants. You usually need to wait several months for the bone to heal completely and finish any necessary radiation therapy before the dentist can place the implants.
What happens if the free flap fails?
While flap failure is rare, it usually occurs within the first 48 hours due to a blood clot. If the surgeon cannot save the flap by clearing the clot in the operating room, they will remove the failed tissue. They will then plan a second reconstruction using a different donor site or a simpler tissue flap once you are stable.
When can I return to work after head and neck reconstruction?
Most patients need at least two to three months of recovery before returning to work. The exact timeline depends on the physical demands of your job and whether you need additional treatments like radiation therapy. You should wait until your energy levels return and your doctor clears you for normal activities.
Learn more about Head & Neck Cancer Surgery
View treatments, doctors & FAQs
Concerned about this condition?
Our specialists can help. Book a consultation today.
Book Consultation
MBBS, MS (ENT), DNB (ENT), MCh (Head & Neck), FICRS, FEB – ORL HNS, ASOHNS
Clinical Director & Senior Consultant Surgeon