In this article
- What is Transoral Robotic Surgery and Laser Treatment?
- Who Needs Transoral Robotic and Laser Surgery?
- How Transoral Robotic Surgery and Laser Treatment is Performed
- Preparing for Robotic and Laser Throat Surgery
- Recovery After TORS and Transoral Laser Surgery
- Risks and Complications
- Results and Success Rate
- Why Choose THANC Hospital for Transoral Robotic and Laser Surgery?
- Frequently Asked Questions

What is Transoral Robotic Surgery and Laser Treatment?
When you receive a diagnosis of throat cancer, understanding your treatment options can feel overwhelming. In the past, surgeons had to perform major open surgeries to reach tumors in the throat and voice box. These traditional methods often required splitting the jawbone or making large incisions across the neck. Today, medical advancements offer minimally invasive alternatives. Two of the most effective methods are Transoral Robotic Surgery (TORS) and Transoral Laser Microsurgery (TLM).
"Transoral" simply means that the surgeon operates entirely through your mouth. Because the surgeon reaches the tumor through your natural airway, you do not need any external cuts on your face or neck. This approach protects your healthy tissue and significantly speeds up your healing process.
Transoral Robotic Surgery uses advanced robotic technology to remove tumors. The surgeon sits at a computer console near your operating table. From this console, the surgeon controls tiny, highly flexible robotic arms that hold surgical instruments. A high-definition 3D camera provides a magnified view of the back of your throat. The robotic system translates the surgeon's hand movements into precise, steady actions inside your mouth. This technology allows the surgeon to navigate tight spaces and remove tumors that were once considered too difficult to reach safely.
Transoral laser treatment takes a slightly different approach but shares the same goal. During this procedure, the surgeon uses a high-powered surgical microscope to view the tumor. Instead of traditional scalpels, the surgeon uses a precise carbon dioxide laser beam. The laser acts as an extremely sharp, bloodless knife. It vaporizes or cuts away the cancerous tissue while simultaneously sealing small blood vessels. This sealing action minimizes bleeding and keeps the surgical area clear.
Both TORS and transoral laser procedures solve major problems for patients with head and neck cancers. They allow surgeons to remove the cancer completely while preserving your ability to speak, swallow, and breathe naturally. By avoiding large neck incisions, these procedures reduce your hospital stay, lower your risk of infection, and help you return to your normal life much faster than traditional open surgery.
Who Needs Transoral Robotic and Laser Surgery?
Surgeons primarily use these minimally invasive procedures to treat cancers located in the throat and voice box. Your doctor may recommend these surgeries if you have tumors in the pharynx (throat), larynx (voice box), tonsils, or the base of your tongue. These areas play a important role in how you eat and speak, making precise surgery absolutely essential.
Head and neck cancers are a major health concern in India. According to recent medical data, head and neck cancer accounts for nearly 30% of all cancer cases in the country. Furthermore, experts project that India will see 2.1 million new cancer cases by 2040. This high prevalence is strongly linked to common lifestyle habits.
Several specific risk factors make these cancers more common among Indian patients:
- Chewing smokeless tobacco products like gutka, khaini, and paan.
- Chewing supari (areca nut), which is a known cancer-causing substance.
- Smoking cigarettes or beedis.
- Heavy and regular alcohol consumption.
- Infection with the Human Papillomavirus (HPV), which is an emerging cause of throat cancer in younger adults.
You can learn more about how these habits affect your mouth by reading about oral cancer early signs and symptoms.
Conservative treatments like radiation therapy or chemotherapy are not always enough to cure these cancers. Sometimes, a tumor does not respond well to radiation. In other cases, a patient may have already received the maximum safe dose of radiation for a previous issue. Surgeons also use TORS and transoral laser surgery as a first step to remove the bulk of a tumor. Removing the tumor first can reduce the amount of radiation or chemotherapy you might need later. You can explore more about these full treatment plans in our guide to throat cancer types, stages, and treatment.
Ideal candidates for these procedures usually have early-stage tumors (Stage I or Stage II). The tumor must be small enough and positioned in a way that the surgeon can clearly see and reach it through the open mouth. Additionally, you must be healthy enough to undergo general anaesthesia. If you have a very large tumor that has spread deeply into the neck muscles or bones, you may still require traditional open surgery. Your surgical team will carefully evaluate your specific condition to determine if you are a good candidate.
How Transoral Robotic Surgery and Laser Treatment is Performed
Understanding the steps of your surgery can help reduce your anxiety before the big day. Both TORS and transoral laser surgeries take place in a fully equipped operating room. You will receive general anaesthesia, meaning you will be completely asleep and pain-free throughout the entire procedure.
Once you are asleep, the surgical team positions you carefully on the operating table. The surgeon places a special mouth retractor between your teeth. This device keeps your mouth open wide and protects your teeth and lips during the surgery. From this point, the steps differ slightly depending on which technology your surgeon uses.
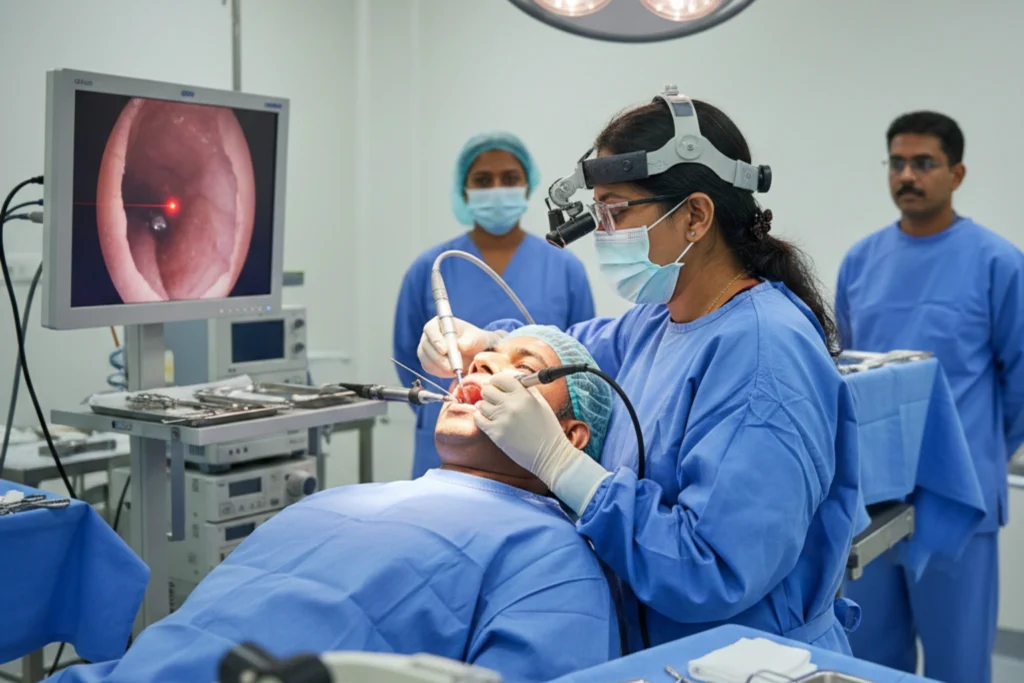
If you are undergoing Transoral Robotic Surgery, the team brings the robotic cart to the side of your bed. The surgeon inserts the 3D camera and the tiny robotic instruments through your mouth. The surgeon then sits at the control console a few feet away. Looking through the console's screen, the surgeon sees a highly magnified, three-dimensional view of your throat. As the surgeon moves their hands at the console, the robotic arms mimic these exact movements inside your throat. The robotic wrists can rotate 360 degrees, providing a range of motion that human hands simply cannot achieve in such a small space. The surgeon carefully cuts the tumor away from the healthy tissue and removes it through your mouth.
If you are having transoral laser surgery, the setup is different. The surgeon positions a powerful surgical microscope over your mouth to get a clear, magnified view of the tumor. The surgeon then directs a precise carbon dioxide laser beam through the microscope. The laser cuts through the tissue to free the tumor. Because the laser seals blood vessels as it cuts, the surgeon maintains a very clear view of the tumor's edges. The surgeon removes the cancerous tissue piece by piece or in one solid block, depending on the tumor's size and location.
After removing the tumor, the surgeon carefully checks the remaining tissue. They want to ensure they have achieved "clear margins," meaning no cancer cells remain at the edges of the surgical site. The surgeon stops any minor bleeding using heat or small clips. Because the surgery happens inside the throat, you usually do not need any stitches. The surgical area will heal naturally over time.
The entire procedure typically takes between one and three hours. The exact duration depends on the size and location of your tumor. Because these methods are minimally invasive, your hospital stay is much shorter than with open surgery. Most patients stay in the hospital for just two to four days before going home to continue their recovery.
Preparing for Robotic and Laser Throat Surgery
Proper preparation is vital for a smooth surgery and a successful recovery. Your medical team will guide you through a series of steps in the weeks and days leading up to your procedure. Following their instructions closely will help minimize your risks and ensure your body is ready to heal.
First, you will need to undergo several pre-operative tests. These tests give your surgeon a complete picture of your health and the exact details of your cancer.
- A biopsy confirms the type of cancer cells present.
- Imaging tests like Computed Tomography (CT) scans or Magnetic Resonance Imaging (MRI) show the size and depth of the tumor.
- A Positron Emission Tomography (PET) scan checks if the cancer has spread to other parts of your body.
- Blood tests and an electrocardiogram (ECG) ensure your heart and organs are strong enough for anaesthesia.
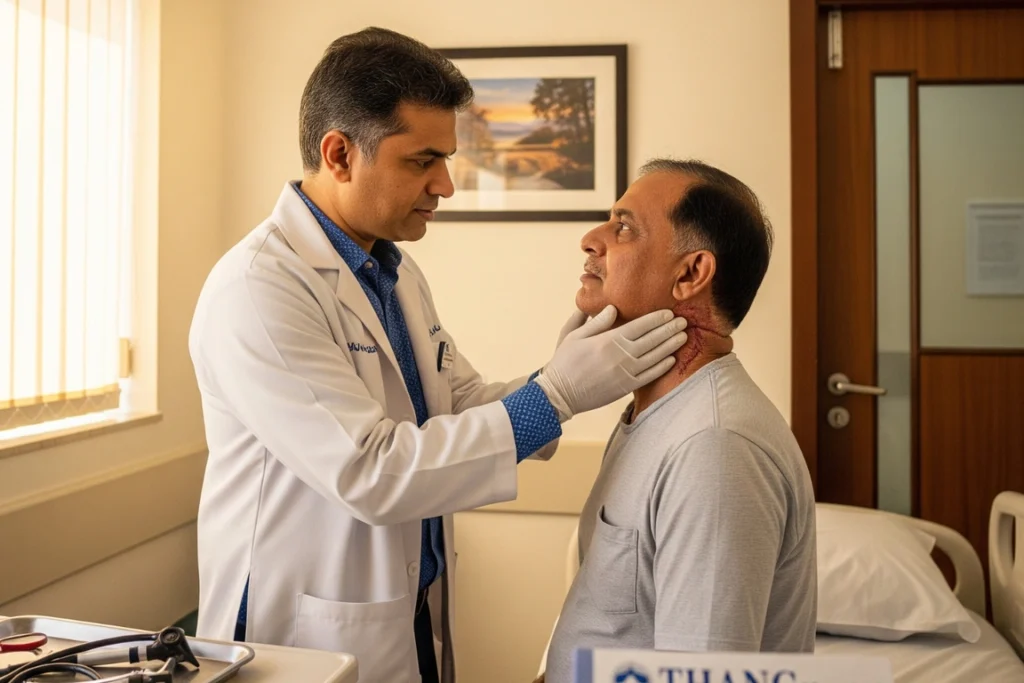
- A vocal cord assessment records your baseline speech and swallowing abilities.
You can read more about the diagnostic process in our detailed article on tongue cancer diagnosis, surgery, and recovery.
Your doctor will also review all the medications you currently take. You must tell your doctor about every pill, supplement, or herbal remedy you use. You will likely need to stop taking blood thinners, such as aspirin or warfarin, several days before surgery to prevent excessive bleeding. If you take medication for diabetes or high blood pressure, your doctor will give you specific instructions on how to manage these on the morning of your surgery.
Lifestyle changes are equally important during this preparation phase. If you smoke or chew tobacco, you must stop immediately. Tobacco use severely restricts blood flow to your tissues, which can delay your healing and increase your risk of infection. Quitting tobacco also lowers your risk of the cancer returning later. You should also avoid alcohol in the days leading up to your procedure.
On the day before your surgery, you will need to fast. This means you cannot eat or drink anything, including water, for at least eight hours before your scheduled arrival time. Fasting prevents complications with the anaesthesia.
When you come to the hospital, bring comfortable, loose-fitting clothes. Bring your personal identification, your health insurance cards, and a folder with all your medical records and test results. You should also expect to wake up with a sore throat. Your medical team may place a temporary feeding tube through your nose to help you get nutrition while your throat begins to heal. Knowing this in advance can help you feel calmer when you wake up in the recovery room.
Recovery After TORS and Transoral Laser Surgery
The recovery process requires patience and careful attention to your body. Because the surgery takes place inside your throat, eating, drinking, and speaking will feel different for a while. Your medical team will support you through each stage of your healing journey.
During the first 24 to 48 hours, you will stay in the Intensive Care Unit (ICU) or a high-dependency ward. Nurses will monitor your breathing, heart rate, and blood pressure closely. You will experience a sore throat, similar to a severe case of tonsillitis. Your doctors will provide strong pain medication through an intravenous (IV) line to keep you comfortable. You will likely have a nasogastric tube (a thin tube running from your nose to your stomach). This tube delivers liquid nutrition and medications directly to your stomach, protecting your surgical site from food particles and preventing you from choking.
Your week-by-week recovery timeline will look something like this:
Week 1: Your primary focus is resting and managing pain. You will remain on a strict liquid diet. Your doctor will advise you to rest your voice completely. You should avoid clearing your throat or coughing forcefully, as this can disrupt the healing tissue.
Weeks 2 and 3: Your throat will start to feel better, and your doctor may remove your feeding tube. You will transition to a soft diet. A Speech-Language Pathologist (SLP) will teach you swallowing exercises to help your throat muscles work properly again. You can also begin using your voice gently for short periods.
Weeks 4 to 6: Your energy levels will return, and your pain will significantly decrease. You can gradually reintroduce more solid foods into your diet. Most patients can return to work and resume light physical activities during this time. Your voice and swallowing function will continue to improve with daily practice.
Dietary restrictions are a important part of your recovery, especially for Indian patients accustomed to flavorful meals. You must avoid spicy curries, acidic foods like pickles or citrus fruits, and rough textures like papad or hard roti. These foods can irritate your healing throat and cause severe pain. Instead, focus on soft, bland, and nutritious Indian foods. Excellent options include soft khichdi, idli soaked in mild sambar, mashed vegetables, smooth dal soup, and plain yogurt. Ensure all your food is lukewarm, as very hot meals can increase swelling in your throat.
You can usually return to your normal daily activities within three to four weeks. However, you should avoid heavy lifting, strenuous exercise, and straining for at least six weeks. Always follow your surgeon's specific timeline, as everyone heals at their own pace.
Risks and Complications
Every surgical procedure carries some level of risk, even minimally invasive ones. Understanding these risks helps you make an informed decision about your treatment. Your surgical team takes extensive precautions to keep you safe, but you should be aware of potential side effects.
Common, minor risks include:
- A severe sore throat that lasts for a few weeks.
- Temporary voice changes, such as hoarseness or a breathy tone.
- Mild difficulty swallowing, known medically as dysphagia.
- Minor bleeding from the surgical site.
- Ear pain, which is actually referred pain from your healing throat.
- Slight chipping of your teeth or numbness in your tongue caused by the mouth retractor.
Rare but serious risks require immediate medical attention. These include:
- Hemorrhage: Severe bleeding from the surgical site can occur if a blood vessel opens up. This is a medical emergency that may require a return to the operating room.
- Airway swelling: Inflammation in your throat can make breathing difficult. In very rare cases, the surgeon may need to perform a temporary tracheostomy (creating a small breathing hole in your neck) until the swelling goes down.
- Aspiration: This happens when food or liquid accidentally enters your lungs instead of your stomach, which can lead to pneumonia.
- Infection at the surgical site, which requires antibiotic treatment.
At THANC Hospital, we take every possible step to minimize these risks. Our surgical team conducts rigorous pre-operative planning using advanced imaging to map out your exact anatomy. We carefully select patients to ensure that robotic or laser surgery is the safest option for their specific tumor. During the procedure, our surgeons use the high-definition magnification of the robot and microscope to protect your healthy blood vessels and nerves. After surgery, our dedicated ICU staff monitors your airway and swallowing function around the clock to catch and treat any complications immediately.
Results and Success Rate
When considering robotic surgery for throat cancer, patients often want to know what kind of outcomes they can expect. The success rates for TORS and transoral laser surgery are highly encouraging, especially for patients with early-stage cancers.
For Stage I and Stage II throat and voice box cancers, these minimally invasive procedures offer excellent cure rates. The primary goal is always to remove the cancer completely. Because the robotic and laser systems provide such clear, magnified views, surgeons can achieve clear margins with high precision. This precision significantly reduces the chance of the cancer returning in the same spot.
Beyond curing the cancer, the functional results are a major advantage. Traditional open surgeries often leave patients with permanent speech impediments or a lifelong reliance on feeding tubes. In contrast, TORS and TLM are designed to preserve your natural anatomy. Most patients regain their normal speaking voice and can eat a regular diet after completing their recovery and swallowing therapy.
The results of your surgery are often permanent, provided the surgeon removes all the cancerous tissue. However, head and neck cancers have a risk of recurrence, or coming back. To ensure your results last, you must attend regular follow-up appointments. Your doctor will perform routine physical exams and imaging tests to monitor your throat. Most importantly, you must permanently stop using all tobacco products and limit your alcohol intake. Continuing these habits drastically increases your risk of developing a new cancer in the future.
Why Choose THANC Hospital for Transoral Robotic and Laser Surgery?
Choosing the right hospital and surgical team is a key decision in your cancer journey. At THANC Hospital, our dedicated Head & Neck Surgery department offers patient-focused care.
Our surgical team is led by Dr. Vidhyadharan S, a highly specialized Head & Neck Surgical Oncologist. Dr. Vidhyadharan possesses extensive expertise and high-volume experience in performing Transoral Robotic Surgery and Transoral Laser Microsurgery. His deep understanding of microvascular reconstruction and swallowing preservation so that you receive the most effective treatment while maintaining your quality of life. If you or a loved one are facing a throat cancer diagnosis, we encourage you to Book an Appointment to discuss your minimally invasive surgical options.
Frequently Asked Questions
Is robotic surgery for throat cancer painful?
You will not feel any pain during the procedure because you will be under general anaesthesia. However, you will experience a severe sore throat for the first week or two of your recovery. Your medical team will provide strong, effective pain medications to keep you comfortable while your throat heals.
Will I lose my voice after transoral laser surgery?
No, you will not permanently lose your voice. You may experience temporary hoarseness or a breathy voice due to swelling in your voice box immediately after surgery. With proper vocal rest and guidance from a speech therapist, your natural voice usually returns within a few weeks.
How long does it take to swallow normally after TORS?
Most patients can swallow liquids safely within the first week after surgery. Transitioning to soft foods takes about two to three weeks, and returning to a completely normal diet usually takes four to six weeks. A swallowing specialist will teach you specific exercises to speed up this process and prevent choking.
Is robotic surgery better than radiation for throat cancer?
Neither treatment is universally "better," as the best choice depends on your specific tumor size, location, and overall health. However, robotic surgery can often remove the tumor entirely in one day, potentially sparing you from the long-term side effects of heavy radiation. Your oncology team will help you decide which approach offers the highest cure rate for your specific case.
Can I eat normal Indian food after throat cancer surgery?
Eventually, yes, but you must modify your diet during the first month of recovery. You need to avoid spicy curries, acidic pickles, and rough foods like hard roti that can irritate your healing throat. You should focus on soft, mild foods like khichdi, idli, and mashed vegetables until your surgeon clears you to resume your regular diet.
Learn more about Head & Neck Surgery
View treatments, doctors & FAQs
Concerned about this condition?
Our specialists can help. Book a consultation today.
Book Consultation